Routine eye exams do more than just update your glasses prescription – they can detect serious eye diseases early, often before symptoms appear. Conditions like glaucoma, cataracts, diabetic retinopathy, and macular degeneration can cause irreversible vision loss if left untreated. Regular screenings also help identify systemic health issues like diabetes and high blood pressure. Here’s a quick look at seven common eye diseases that can be identified during routine exams:
- Glaucoma: Silent damage to the optic nerve, often detected through tonometry, pupil dilation, and OCT imaging.
- Cataracts: Cloudy lenses diagnosed with visual acuity tests and slit-lamp exams.
- Macular Degeneration: Affects central vision; detected using OCT and fluorescein angiography.
- Diabetic Retinopathy: Retinal damage from diabetes, identified via dilated exams and retinal imaging.
- Dry Eye Syndrome: Diagnosed by examining tear film quality and meibomian glands.
- Retinal Detachment: A medical emergency spotted with dilated exams and imaging tools like OCT or ultrasound.
- Thyroid Eye Disease: Linked to autoimmune issues, identified through physical exams and imaging.
Early detection is key to preserving vision. Even if your vision feels fine, schedule regular eye exams to catch these conditions early and protect your overall health.
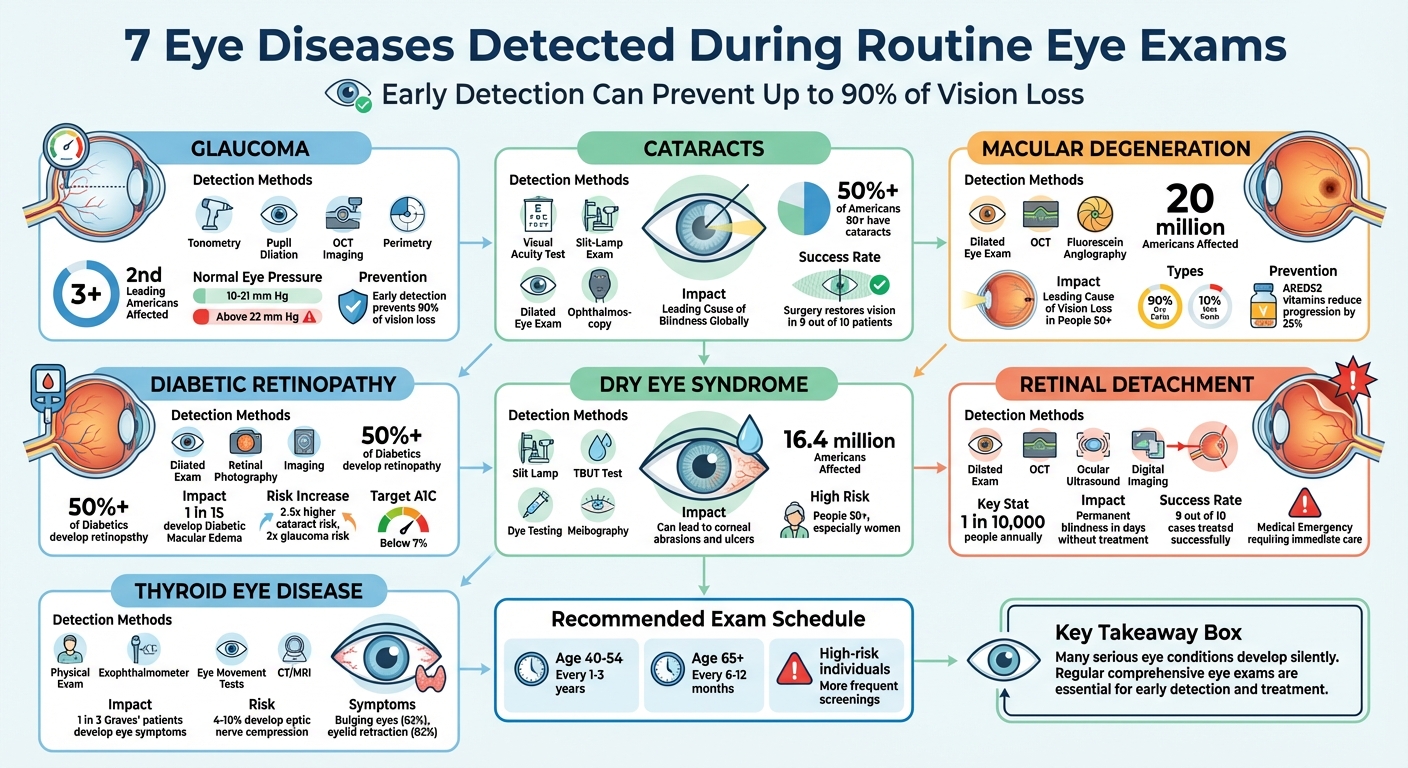
7 Eye Diseases Detected During Routine Eye Exams: Detection Methods and Impact
1. Glaucoma
Detection Methods During Routine Eye Exams
Glaucoma often develops silently, showing no symptoms until significant damage has occurred. During routine eye exams, several tests can identify the condition early. Tonometry, for instance, measures eye pressure. Normal levels range from 10 to 21 mm Hg, and anything above 22 mm Hg could signal a potential risk. Pupillary dilation allows doctors to examine the optic nerve for signs of damage, such as cupping or color changes. Another essential test is perimetry, which maps peripheral vision to detect any unnoticed blind spots.
Other advanced methods provide deeper insights. Gonioscopy examines the drainage angle between the iris and cornea to differentiate between open-angle and closed-angle glaucoma. Pachymetry measures corneal thickness, which is significant because thinner corneas can obscure high eye pressure readings. Additionally, Optical Coherence Tomography (OCT) generates detailed 3D images of the optic nerve and retinal nerve fiber layer, making it easier to track subtle changes over time. These tools collectively provide a comprehensive picture of eye health, ensuring accurate detection and management.
Understanding these diagnostic methods is vital, as glaucoma often progresses unnoticed, threatening vision if left untreated.
Impact on Vision and Eye Health
Glaucoma damages the optic nerve, which transmits visual signals from the retina to the brain. The condition typically starts with peripheral vision loss, often near the nose, and progresses so gradually that many people remain unaware of it until the disease is advanced. In the U.S., glaucoma affects over 3 million people and is the second leading cause of blindness.
"Patients with POAG most commonly experience no symptoms at all until the disease progresses to an advanced stage." – Yvonne Ou, MD, Professor of Ophthalmology, University of California, San Francisco
If untreated, glaucoma can lead to complete blindness. Beyond vision loss, advanced stages increase the likelihood of falls, injuries, and even psychological challenges like social isolation and depression. Unfortunately, the damage caused by glaucoma is permanent; once optic nerve fibers are destroyed, they cannot regenerate.
Importance of Early Diagnosis and Treatment
Catching glaucoma early can prevent up to 90% of vision loss caused by the disease. While there is no cure, treatments to lower eye pressure – such as prescription eye drops, laser procedures like Selective Laser Trabeculoplasty (effective in 75–80% of cases), or surgery – can significantly slow or halt further damage.
"Early diagnosis is critical… When you take control of your health, by getting regular eye exams and beginning an appropriate treatment plan, you are less likely to have significant vision loss from glaucoma." – Cheyenne Eye Clinic & Surgery Center
The American Academy of Ophthalmology advises adults aged 40 to 54 to have comprehensive eye exams every one to three years, while those aged 65 and older should schedule exams every six to 12 months. Individuals at higher risk – such as African Americans over 40, Hispanic/Latino individuals over 60, or those with a family history of glaucoma – should consider more frequent screenings. Waiting for symptoms is risky, as irreversible damage may have already occurred by the time they’re noticeable.
Consistent glaucoma screenings are vital for protecting your vision and preserving your overall quality of life.
sbb-itb-246add9
2. Cataracts
Detection Methods During Routine Eye Exams
Cataracts are identified during routine eye exams using specific tests designed to evaluate the clarity of your lens. They develop when proteins in the lens break down, creating cloudy areas that block light from reaching the retina properly.
A visual acuity test checks how well you can see at various distances, typically using a standard letter chart. The slit-lamp exam employs a special microscope and bright light to closely examine the lens, cornea, and iris, revealing details like the size and location of cloudiness. During a dilated eye exam, your doctor will use drops to enlarge your pupils, which helps assess the severity of cataracts and detect any related retinal issues. Another tool, ophthalmoscopy, allows for a detailed look at the back of the eye, helping to identify specific types of cataracts, such as posterior subcapsular cataracts. These methods confirm the diagnosis and help determine how much the condition is affecting your vision.
Impact on Vision and Eye Health
Cataracts are the leading cause of blindness in both the United States and across the globe. In fact, more than half of Americans aged 80 or older either have cataracts or have undergone surgery to remove them.
This condition gradually diminishes vision. Common symptoms include increased sensitivity to light, glare, and seeing halos or streaks around lights – issues that are particularly troublesome when driving at night. As the lens becomes less flexible and more opaque, colors may appear dull, and reading can become increasingly challenging. If left untreated, cataracts can eventually result in complete vision loss.
Importance of Early Diagnosis and Treatment
Catching cataracts early makes a big difference in treatment outcomes. Early detection allows for managing symptoms with practical solutions like brighter lighting, anti-glare sunglasses, or updated prescriptions before the condition starts to disrupt daily life. If surgery becomes necessary, addressing the issue in its earlier stages often leads to better results and improved vision.
"Cataract surgery is one of the most common operations in the United States" – National Eye Institute
Timely surgery can restore vision for 9 out of 10 patients. Adults over 40 should schedule regular comprehensive eye exams that include dilation, and those aged 60 or older should be checked every one to two years. If you notice symptoms like cloudy vision, faded colors, or difficulty driving at night, consult your eye doctor right away. Additionally, wearing UV-protective sunglasses and managing conditions like diabetes can help slow the progression of cataracts.
3. Macular Degeneration
Detection Methods During Routine Eye Exams
Macular degeneration, much like glaucoma and cataracts, can progress silently, making early detection crucial. At Cheyenne Eye Clinic and Surgery Center, advanced techniques are employed to catch the condition in its early stages. A routine eye exam typically includes a dilated eye exam, where eye drops are used to widen the pupils. This helps the doctor examine the retina and macula for signs of drusen – tiny deposits that point to early dry macular degeneration. Another key tool is Optical Coherence Tomography (OCT), which uses light waves to create detailed cross-sectional images of the retina, revealing issues like macular thinning or fluid buildup. For wet macular degeneration, fluorescein angiography may be performed. This involves injecting dye into the bloodstream to highlight any leaking blood vessels. These methods work together to provide a comprehensive assessment of central retinal health.
Impact on Vision and Eye Health
Macular degeneration targets the macula, the part of the eye responsible for sharp central vision. In the U.S., about 20 million adults are affected, making it a leading cause of vision problems in people over 50. Symptoms can start subtly, with blurry or wavy vision, but the condition can eventually lead to severe central vision loss. The "dry" form accounts for nearly 90% of cases and involves gradual retinal thinning and drusen buildup. The remaining 10% are "wet" cases, marked by rapid fluid or blood leakage from abnormal blood vessels. While peripheral vision often remains intact, losing central vision can result in legal blindness and may also lead to emotional challenges like depression and anxiety.
Importance of Early Diagnosis and Treatment
Catching macular degeneration early is key to slowing its progression, as damage to the macula is generally permanent. Although there’s no cure, early diagnosis opens the door to treatments that can make a meaningful difference. For example, the AREDS2 vitamin formula – which includes vitamins C and E, zinc, copper, lutein, and zeaxanthin – has been shown to reduce the risk of progression in intermediate cases by about 25%. For wet macular degeneration, anti-VEGF injections can help prevent rapid vision loss when administered promptly. Regular annual exams and tools like the Amsler grid for home monitoring allow for quick action if new symptoms, such as wavy lines or dark spots, arise.
What Doctors Can Tell About Your Health From A Routine Eye Exam | Eye Surgeons Associates
4. Diabetic Retinopathy
Diabetic retinopathy is a hidden danger that can be identified through thorough eye exams. In its early stages, this condition often develops without any noticeable symptoms, which is why regular eye check-ups are essential to catch it before it causes permanent harm [29, 30]. During an exam, dilation – using eye drops to widen your pupils – allows specialists to closely examine the retina, optic nerve, and blood vessels. They look for signs like microaneurysms (tiny bulging blood vessels), retinal hemorrhages (bleeding in the retina), cotton wool spots, and abnormal growth of new blood vessels [28, 29, 30]. In more advanced cases, imaging techniques and retinal photography are used to monitor the disease’s progression. As with many conditions, early detection during routine exams is key to managing diabetic retinopathy effectively.
Impact on Vision and Eye Health
The silent nature of diabetic retinopathy makes early diagnosis critical. High blood sugar over time damages the small blood vessels in the retina, leading to two distinct stages of the disease. In the early stage, known as nonproliferative diabetic retinopathy (NPDR), blood vessels may leak or close off, resulting in issues like microaneurysms and cotton wool spots. These might go unnoticed or cause mild blurriness if macular edema develops. The more severe proliferative diabetic retinopathy (PDR) stage occurs when fragile new blood vessels form on the retina. These vessels can bleed into the vitreous, increasing the risk of severe vision loss, retinal detachment, and even permanent blindness [29, 31].
Statistics show that over half of people with diabetes will develop some form of retinopathy over time. Around 1 in 15 will experience Diabetic Macular Edema (DME), where fluid leaks into the macula, leading to blurred central vision. Diabetes also raises the risk of cataracts by 2 to 5 times and nearly doubles the likelihood of developing open-angle glaucoma.
Importance of Early Diagnosis and Treatment
"The sooner you detect diabetes-related eye diseases, the more likely you are to prevent or delay vision loss." – American Diabetes Association
Early detection is essential for protecting your vision. If you have Type 2 diabetes, schedule a comprehensive eye exam as soon as you’re diagnosed, as eye damage may already be present [28, 30]. For those with Type 1 diabetes, it’s recommended to have a dilated eye exam within five years of diagnosis and then continue with annual exams [28, 30]. Pregnant women with diabetes should have an eye exam before pregnancy or during the first trimester, as pregnancy can accelerate or worsen retinopathy [28, 30].
Beyond regular exams, managing your overall health plays a big role in slowing retinal damage. Aim to keep your A1C level below 7% and maintain blood pressure under 130/80 [30, 34, 38]. If you notice sudden changes like floaters, flashes, dark spots, or blurred vision, seek immediate medical attention [30, 31].
5. Dry Eye Syndrome
Detection Methods During Routine Eye Exams
Dry eye syndrome impacts about 16.4 million Americans, and a comprehensive eye exam can help identify it early on. During the exam, your eye doctor might use a slit lamp to examine your eyelids, conjunctiva, and tear film for any inflammation or blockages in the meibomian glands, which are crucial for maintaining the tear film’s oily layer. Additional tests like the Tear Break-Up Time (TBUT) test, dye testing with Sodium Fluorescein or Lissamine Green, meibography, and tear volume assessments provide a detailed evaluation to confirm the condition before symptoms worsen.
Interestingly, watery eyes can also be a sign of dry eye syndrome. This happens when the body compensates for poor-quality tears by producing reflex tears. Other symptoms often include stringy mucus, a gritty feeling, burning, redness, light sensitivity, and temporary blurred vision that clears up after blinking.
Impact on Vision and Eye Health
Without treatment, dry eye syndrome can progress from being mildly uncomfortable to posing serious risks to your vision. Severe cases may lead to chronic inflammation, corneal abrasions, or even ulcers, all of which have the potential to cause permanent vision loss. The condition can also interfere with everyday tasks like reading or driving due to fluctuating vision and increased sensitivity to light. People over 50, especially women, are at a higher risk of developing this condition.
Importance of Early Diagnosis and Treatment
Catching dry eye syndrome early is essential for avoiding long-term damage. Routine exams help your doctor pinpoint which part of your tear film – oily, watery, or mucus – is lacking, allowing for targeted treatments before the glands experience irreversible damage. Early detection can also reveal underlying health issues like Sjögren’s syndrome, thyroid disease, lupus, or rheumatoid arthritis.
Managing symptoms often starts with simple lifestyle changes. Using a humidifier, wearing wraparound sunglasses, lowering screen height, applying warm compresses, and increasing omega-3 intake can help reduce tear evaporation and support gland function. If you notice persistent redness, irritation, or eye fatigue, it’s a good idea to book a comprehensive eye exam to get a proper diagnosis.
6. Retinal Detachment
Detection Methods During Routine Eye Exams
Retinal detachment is one of those silent threats to vision that demands swift action. A dilated eye exam is the go-to method for spotting it. This involves using eye drops to widen your pupils, allowing your doctor to get a clear look at the retina at the back of your eye. To dig deeper, your doctor might use tools like ophthalmoscopy to inspect the retina and blood vessels or perform scleral depression, which involves gently pressing on the eyelids to get a better view of the peripheral retina – where small tears often hide.
In addition to the dilated exam, advanced testing methods can provide even more clarity. OCT (Optical Coherence Tomography) delivers detailed cross-sectional images of the retina. Ocular ultrasound comes in handy when the view is blocked by factors like cataracts or bleeding. And digital retinal imaging captures wide-angle photos, making it easier to spot changes over time.
Impact on Vision and Eye Health
Retinal detachment is a serious condition because it cuts the retina off from its blood supply, which is vital for vision. Symptoms often appear suddenly and can include a surge in floaters, flashes of light, or the ominous presence of a dark "curtain" creeping across your vision. The National Eye Institute stresses the urgency of this situation:
"Retinal detachment is a medical emergency. If you have symptoms of a detached retina, it’s important to go to your eye doctor or the emergency room right away".
The stakes are high. Without immediate treatment, the damage can escalate quickly. According to Cleveland Clinic:
"Permanent blindness can happen as quickly as a few days".
In the U.S., retinal detachment affects about 1 in 10,000 people annually, with the risk for the most common type ranging between 6.3 and 17.9 per 100,000 individuals.
Importance of Early Diagnosis and Treatment
Catching retinal detachment early can make all the difference. Surgery has a high success rate – about 9 out of 10 cases are treated effectively . If the detachment is spotted before it reaches the macula (the part of the retina responsible for sharp vision), the chances of preserving detailed vision are excellent. In cases where only a retinal tear is present, less invasive options like laser therapy or cryopexy can seal the tear before it progresses to a full detachment.
The National Eye Institute highlights the importance of routine checks:
"A dilated eye exam can help your eye doctor find a small retinal tear or detachment early, before it starts to affect your vision".
If you notice sudden flashes of light, a burst of new floaters, or a shadow over your vision, don’t wait – seek immediate care. Clinics like Cheyenne Eye Clinic and Surgery Center offer thorough exams aimed at early detection. Regular comprehensive dilated eye exams are especially critical for those who are highly nearsighted, have diabetes, or have a family history of retinal issues. Just like with glaucoma or cataracts, early diagnosis is essential for protecting your vision.
7. Thyroid Eye Disease
Detection Methods During Routine Eye Exams
Thyroid eye disease (TED) impacts around 3 million Americans and can often be identified during a routine eye exam – even before thyroid problems are diagnosed. The process usually begins with a review of your medical history, focusing on thyroid or autoimmune symptoms.
During the physical exam, doctors look for telltale signs like bulging eyes (proptosis) and eyelid retraction, which occur in 62% and 82% of cases, respectively. Swelling or redness around the eyelids may also be noted. To measure the degree of eye bulging, a tool called an exophthalmometer is used [54,55].
Functional tests play a critical role in assessing how well your eyes are working. These tests include checking for restricted eye movements that might cause double vision, evaluating color vision and pupil responses for signs of optic nerve compression, and measuring intraocular pressure [54,55]. Advanced imaging techniques, such as digital retinal photography, ultrasound, CT, or MRI, can confirm muscle enlargement and increased orbital fat [53–55].
Impact on Vision and Eye Health
TED is an autoimmune disorder where the immune system mistakenly attacks tissues behind the eyes, causing inflammation and swelling. It is strongly linked to Graves’ disease, with about one in three Graves’ patients developing eye symptoms. Interestingly, TED symptoms can sometimes appear before thyroid issues are diagnosed, highlighting the importance of routine eye exams. The disease typically follows a pattern called the "Rundle Curve", which includes an active inflammatory phase lasting anywhere from 6 months to 5 years, followed by a stable phase [58,59]. During the active phase, symptoms may include dryness, a gritty sensation, blurry vision, light sensitivity, and double vision.
The National Eye Institute cautions:
"In rare cases, swelling around the eyes can press on the optic nerve… and cause vision loss".
Dysthyroid Optic Neuropathy (DON), which affects 4–10% of TED patients, can compress the optic nerve and lead to permanent vision loss. Smoking is a major risk factor that worsens the disease and makes treatment less effective [58,59]. Smokers often experience an active phase lasting 2 to 3 years compared to about 1 year for non-smokers [54,59].
Importance of Early Diagnosis and Treatment
Early detection of TED is crucial in preventing serious vision complications. Most vision loss occurs during the active inflammatory phase, making timely intervention essential. Treatments like immunomodulators and radiotherapy are most effective when started early. As the Review of Optometry emphasizes:
"Because TAO can precede, coincide with or succeed the diagnosis of thyroid dysfunction, optometrists need to be capable of making an early diagnosis, as TAO can be vision-threatening".
Although only about 5% of patients experience vision loss due to optic nerve compression, prompt treatment can significantly reduce this risk. Early detection also opens the door for lifestyle changes – such as quitting smoking – that can lessen the severity and duration of the disease [54,59]. These patient-driven adjustments can have a meaningful impact on outcomes.
If you have Graves’ disease or a family history of autoimmune disorders, scheduling annual eye exams is essential. Be sure to report any persistent eyelid swelling, redness, or gritty sensations to your eye doctor right away [54,57]. Comprehensive eye exams are a vital tool for catching TED and other conditions early, when treatment is most effective. Clinics like Cheyenne Eye Clinic and Surgery Center offer these exams to ensure conditions like TED are identified and managed promptly.
Conclusion
Regular eye exams are essential for protecting your vision. Many serious eye conditions – like glaucoma, diabetic retinopathy, and macular degeneration – develop quietly, causing irreversible damage before symptoms appear. The good news? Early detection can prevent a significant amount of vision loss. For example, over 3 million Americans have glaucoma, but half of them don’t even know it. Similarly, many cases of diabetic retinopathy are diagnosed too late for treatments to work effectively. These statistics highlight how crucial it is to catch these conditions early.
Comprehensive eye exams are the key to early detection, which allows for timely treatment to preserve vision. Dr. Matthew Bovenzi, Assistant Clinical Professor at SUNY Optometry, emphasizes this point:
"Early detection and treatment of high cholesterol can help avoid potentially blinding or otherwise sight-threatening–and even life-threatening–conditions!"
Symptoms like blurry vision or floaters often mean the disease has already progressed to an advanced stage. That’s why experts recommend scheduling a baseline comprehensive eye exam at age 40, even if your vision seems fine. After age 65, it’s wise to have yearly exams – or more frequently if you have risk factors such as diabetes or high blood pressure.
Cheyenne Eye Clinic and Surgery Center offers a full range of eye care services, from routine exams to advanced treatments for conditions like cataracts, glaucoma, and retinal diseases. Their team of board-certified optometrists and ophthalmologists provides seamless care, from diagnosis to treatment. By scheduling a comprehensive eye exam, you can detect these silent threats early and take steps to protect your vision. Don’t wait – schedule your eye exam today to safeguard your sight and overall health.
FAQs
How often should I get a comprehensive eye exam?
Adults are encouraged to schedule a comprehensive eye exam every 1-2 years. For seniors or those with certain risk factors, more frequent check-ups might be necessary to catch silent eye conditions early and ensure vision stays in good shape. These regular exams play a crucial role in identifying issues such as glaucoma, cataracts, and macular degeneration before they progress.
Which eye diseases can develop without symptoms?
Some eye conditions, such as glaucoma, cataracts, and macular degeneration, can progress silently without obvious symptoms. Routine eye exams play a critical role in identifying these issues early, emphasizing why regular check-ups are essential for maintaining good eye health.
What symptoms mean I need urgent eye care?
If you notice sudden vision loss, intense eye pain, flashes of light, new floaters, or sustain an eye injury, seek immediate eye care. These symptoms could point to serious issues like retinal detachment or glaucoma, which need prompt medical attention.
